Blog
Payer Outages Are Silently Breaking Patient Onboarding. Now You Can See Them
Bridge now gives virtual care teams a live view of payer real-time eligibility system health, so you can stop guessing and start responding.
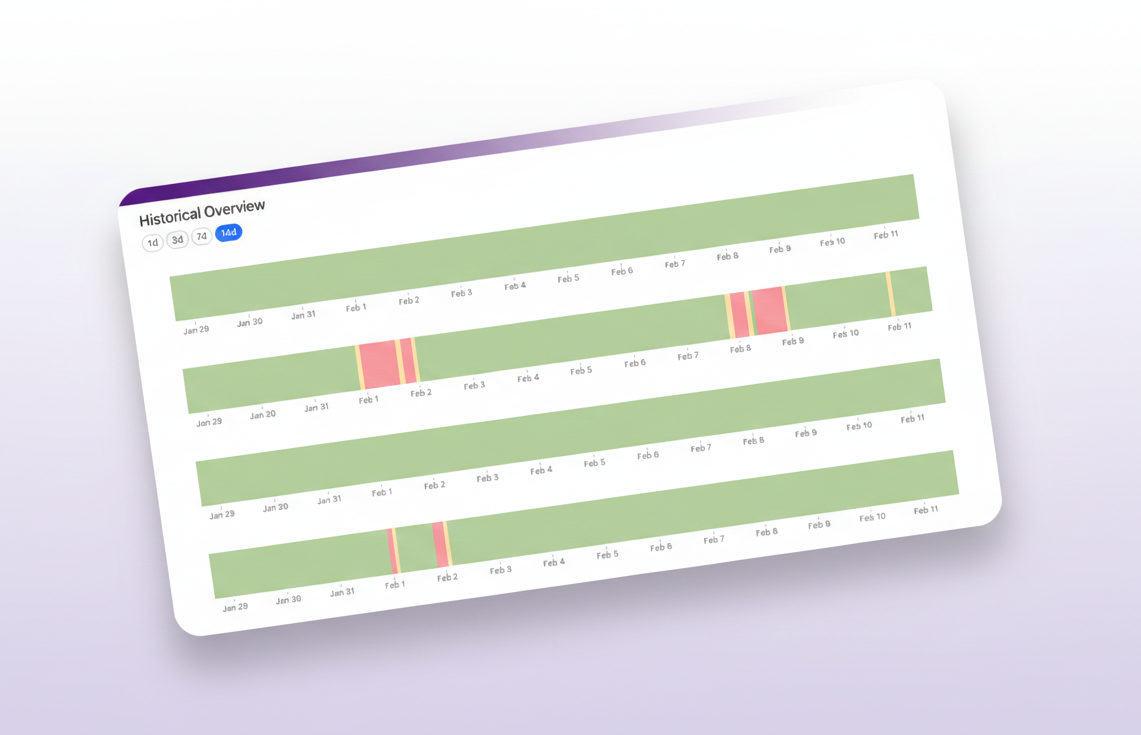
Every ops team running insurance-billed telehealth has been there: it's Sunday night, eligibility requests start failing, and the Slack messages roll in. "Is Blue Cross down right now?" "Are we seeing errors on Aetna or is it just us?"
Payer infrastructure for eligibility verification is notoriously old and unreliable. Systems go down without warning, degrade silently, and leave clinical teams scrambling to figure out whether the problem is on their end or the payer's. Patients get stuck in onboarding limbo. Ops teams burn hours manually verifying coverage. And if you're running paid acquisition, you might be spending money driving patients into a broken funnel without even knowing it.
We built Payer Network Status to fix that.
What We Launched
Bridge processes thousands of eligibility requests every day across our entire partner network. That volume provides a unique, real-time signal on how each major payer group is performing at any given moment.
We're now surfacing that signal directly to our partners through three channels:
- Dashboard: A traffic-light widget lives at the top of every page in the Bridge Dashboard. Green means healthy. Orange or red means a payer is degraded or down. Click through to the Payer Network Status page for an interactive timeline of every health event.
- API: Query current payer status or pull historical health events programmatically. Feed payer reliability data into your internal dashboards, BI tools, or operational workflows.
- Webhooks: Get real-time push notifications the moment a payer's health status changes. No more waiting for a BI refresh or a Slack thread to tell you something's wrong.
Why This Matters
This isn't just a status page. It's operational infrastructure for teams that run on insurance eligibility.
For ops teams, it means instant clarity. When eligibility requests start returning unexpected results, you can immediately see whether it's a payer-side issue—no investigation required. Your team stops wasting cycles diagnosing phantom problems and starts triaging the real ones.
For growth teams, it means smarter spend. Bridge partners can connect our webhooks to their acquisition workflows, automatically pausing ad spend when a major payer goes down and spinning it back up when they're healthy. That's fewer dollars wasted, fewer patients having a broken experience, and less frustration all around.
For engineering teams, it means a building block. The API and webhooks are designed to plug into whatever you've already built: internal dashboards, alerting systems, patient communication workflows. If you've ever wished you had a reliable, real-time signal on payer health, now you do.
From the Field
We heard this pain directly from operators before building it. One team member who previously ran clinical operations at a virtual care company shared their experience:
Our eligibility vendor had a similar status page and it was incredibly helpful. But what we really needed was a real-time push notification system for extended payer outages. Our BI tool only refreshed every four hours, which meant patients could sit in onboarding limbo for hours before we even knew there was a problem. For a well-resourced team, an automated notification on payer errors — combined with automatic re-verification — would have been a game changer. We could have built a faster system ourselves, but we didn't have the resources.
Bridge's Payer Network Status was designed to solve exactly this: real-time webhooks that notify your systems the moment a payer degrades, so no patient is left waiting and no ops team is flying blind.
A Word From Our CTO
We process thousands of eligibility requests a day. At that volume, payer reliability patterns become obvious quickly. The hard part wasn't detecting the signal, it was packaging it in a way that's immediately useful, whether you're an ops lead checking a dashboard or an engineer wiring up a webhook.
- Richard Taylor, Co-founder & CTO at Bridge
How to Get Started
If you're already a Bridge partner, you'll see the status widget in your Dashboard today. Check out the Monitoring Payer Health Guide in our documentation for setup instructions on the API and webhooks.
If you're not yet on Bridge and want to see how real-time payer visibility fits into a full insurance infrastructure — from contracting and credentialing to RCM and compliance — get in touch.
Bridge enables virtual care companies to accept insurance and get in-network nationally in approximately 30 days. Our platform combines payer contracting, provider credentialing, revenue cycle management, and compliance into a single API-driven solution covering 200M+ lives across all 50 states.
.png)